The Ultimate Guide to Restoring Glucose Oxidation
Why carbs aren’t the problem, how to retrain your metabolism to burn them cleanly, and the exact protocol I used to eat 700 g of carbs a day with perfect blood sugar.
If you fix glucose oxidation, you can eat 200–700 g of carbs per day and get calmer, leaner, stronger, with better sleep, higher T3, DHEA-S, IGF-1, and lower cortisol, all without the low-carb crash.
You don’t have a carb problem, you have an oxidation problem. Your PDH is blocked, fatty-acid oxidation (FAO) is dominating, and your redox balance is stuck.
Low-carb “works” … by raising stress hormones and avoiding the real issue. It’s a patch, not a cure. When someone adds carbs back in, they’re still insulin resistant, showing they never solved the problem.
Add carbs on top of that broken system and you get bloat, fatigue, blood sugar spikes, then you blame the carbs instead of your metabolism.
For the last decade, I’ve experimented with everything from high-carb (300–400 g/day) to very low-carb (0–10 g/day) and everything in between.
Right now, I’m eating 700 g of carbs per day for my 20-banana-a-day experiment and my blood sugar is spectacular.
My fasting glucose sits between 70–80 mg/dL, and even after massive carb meals, it rarely exceeds 120–140 mg/dL, often staying under 100 mg/dL.
My fasting insulin and C-peptide are on the lower end of normal, showing superior insulin sensitivity without needing 30k steps a day, HIIT before every meal, or metformin.
My last HbA1c was 4.9.
Carbs aren’t bad. Poor oxidation is.
Here’s what you’ll get from this article:
A step-by-step restoration playbook: how to fix oxidation through food, cofactors, stacks, and timing.
A 14-day Oxidation Reset: exact dosing ranges, meal timing, decision trees, and troubleshooting.
Ready-to-use templates: glucose testing sheets, stack calculator, grocery map, and lab checklist.
Next, we’ll break down why people think carbs are the problem, how poor glucose oxidation sabotages hormones, and how to rebuild your metabolism so carbs start working for you again.
Quick side note here: I’m running an Oct special on Andronaut Academy for 50% off. That’s where I help you dial in your protocol and get your questions answered so that you can start making progress again.
Why This Matters
When you oxidize glucose properly, you get:
Higher thyroid output (T3) → faster metabolism, more energy, better mood.
Higher DHEA-S & free testosterone → more drive, focus, confidence, libido.
Higher IGF-1 → faster recovery, muscle growth, better skin and hair.
Lower cortisol & adrenaline → calmer mind, better sleep, deeper recovery.
In short:
Proper glucose oxidation is what flips you from stressed survival mode to anabolic, high-performing mode.
That’s what this guide is about, not how to eat more carbs, but how to burn them cleanly again.
The Basics: What Happens When You Eat Carbs
Most people think “carbs = sugar = insulin spike,” but what actually happens inside your body is a beautifully coordinated energy delivery system. Here’s how it works step by step:
1. Digestion & Absorption
Glucose and fructose are broken down from starches and sugars (fruit, milk, etc.) in the small intestine.
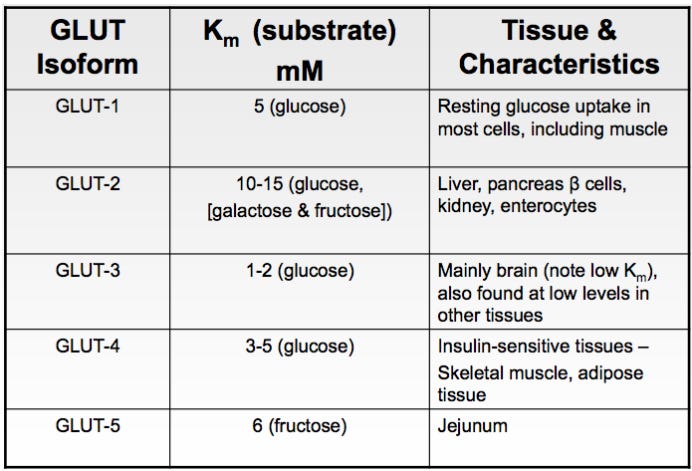
They’re absorbed through specialized transporters:
SGLT1 and GLUT2 move glucose (and galactose) across the intestinal lining.
GLUT5 moves fructose in.
Fructose absorption is slower, which helps smooth blood sugar spikes.
Most of the eaten fructose is converted to glucose inside the intestinal wall before it even reaches the liver.
2. First Stop — The Liver
The absorbed sugars flow directly to the liver through the portal vein.
The liver acts as a glucose buffer, it decides how much to store and how much to release.
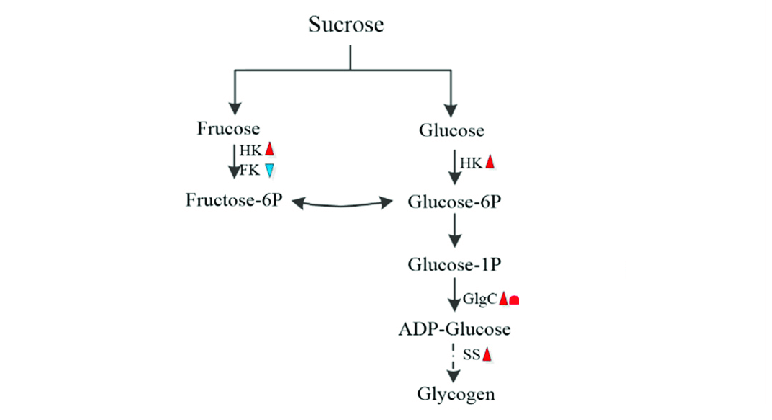
Fructose is mostly handled here; it’s quickly turned into glycogen or glucose, making it the best fuel for refilling liver glycogen.
Glucose is partly stored as liver glycogen, regulated by the enzyme GSK-3β (glycogen synthase kinase-3β; being inhibitory).
When insulin is released from the pancreas, it suppresses GSK-3β, activating glycogen synthase, letting the liver store glucose efficiently.
There are diabetic drugs that inhibit GSK-3β to help lowering circulating glucose and improve insulin sensitivity.
3. Into the Bloodstream & Tissues
The liver releases glucose into circulation.
Insulin tells muscle, fat, and other tissues to take up that glucose via GLUT4 transporters. Glucose can be passively taken up without insulin via the GLUT1 transporter.
Fructose can slip into cells independently of insulin through GLUT5, and interestingly, it can enhance glucose uptake (insulin memetic effect); one reason fruit before starch lowers the glycemic response of a meal.
4. Inside the Cell — Storage or Burning
Once glucose is inside, it has two main fates:
Stored as glycogen for later use.
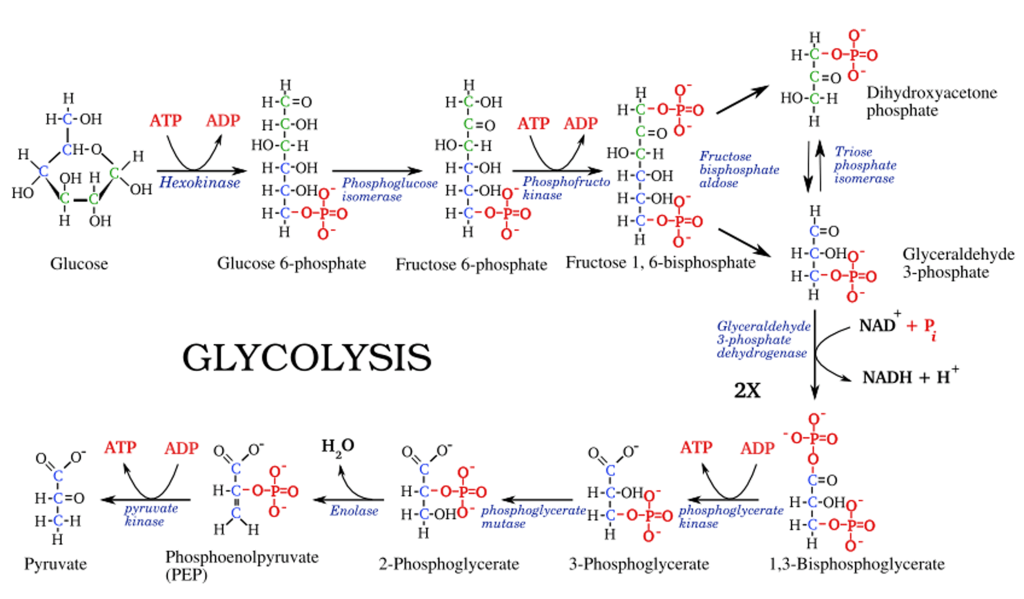
Burned immediately through glycolysis — a 10-step pathway converting glucose → pyruvate.
Glycolysis yields small amounts of ATP and NADH, but the real energy comes later.
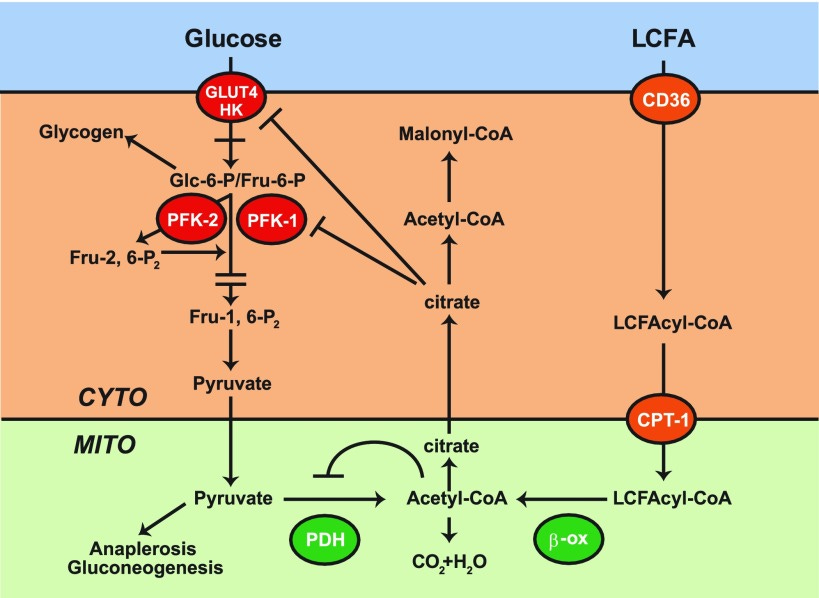
5. The Mitochondrial Gate — Pyruvate Dehydrogenase (PDH)
Pyruvate now has two options:
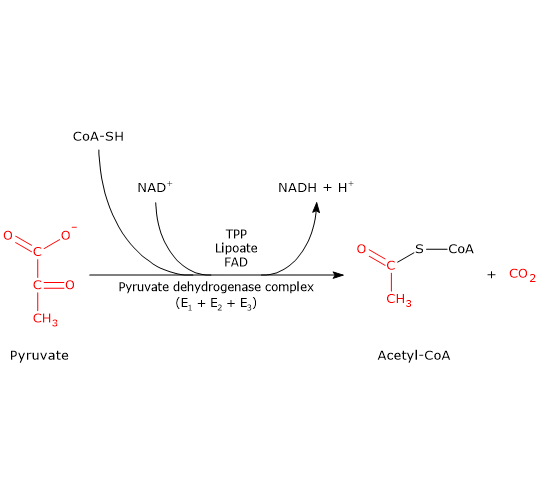
Enter the mitochondria and be converted to acetyl-CoA by pyruvate dehydrogenase (PDH).
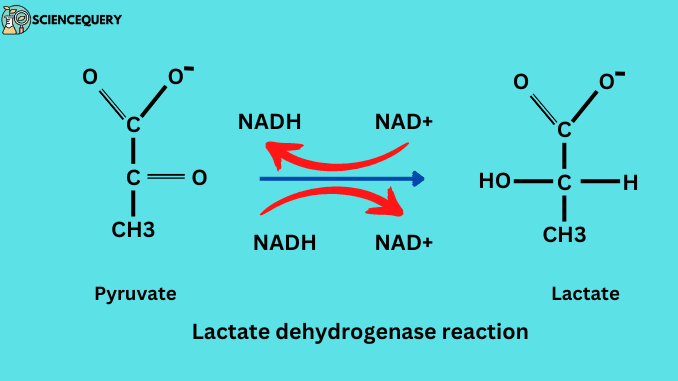
Or, if PDH is inhibited, it’s reduced to lactate instead, recycling NADH back into NAD.
PDH is the key “gatekeeper” of glucose oxidation, it decides whether carbs are burned or fermented (converted to lactate).
PDH activity is limited by:
High NADH/NAD⁺ ratio (redox imbalance)
High ATP (already plenty of energy)
Fatty acid oxidation (Randle cycle inhibition)
When PDH is sluggish, lactate builds up, a sign that glucose is entering the cell but not reaching the mitochondria.
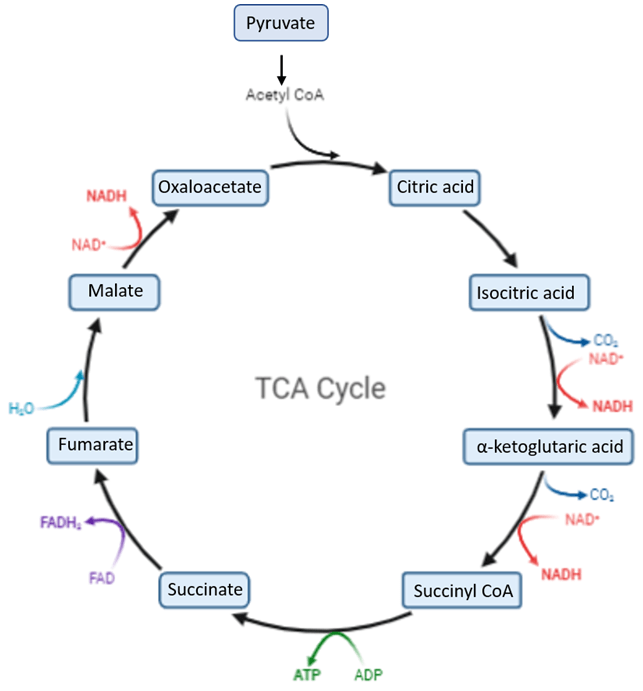
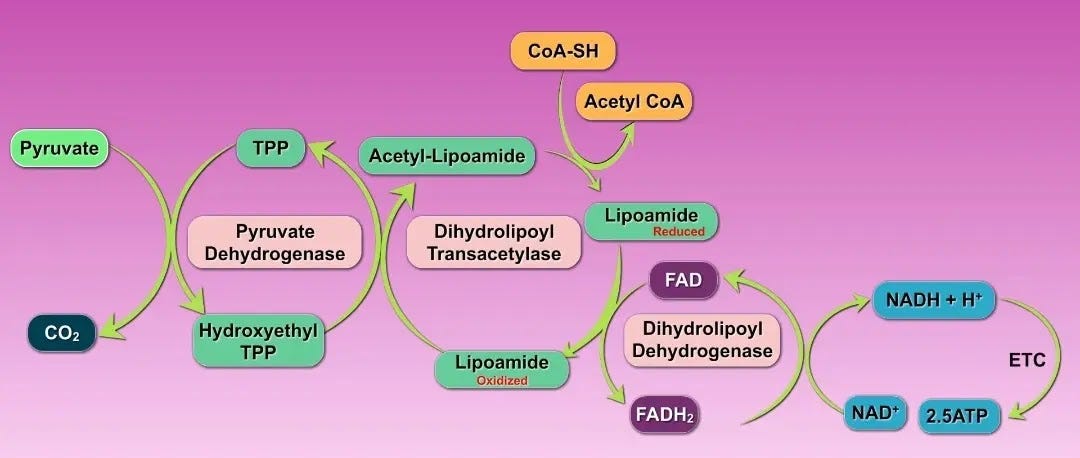
6. The Krebs Cycle (TCA Cycle)
Inside the mitochondria, acetyl-CoA joins with oxaloacetate to begin the Krebs cycle.
Each turn strips hydrogens and electrons, loading them onto NAD⁺ → NADH and FAD → FADH₂.
These high-energy carriers then feed electrons into the electron transport chain (ETC).
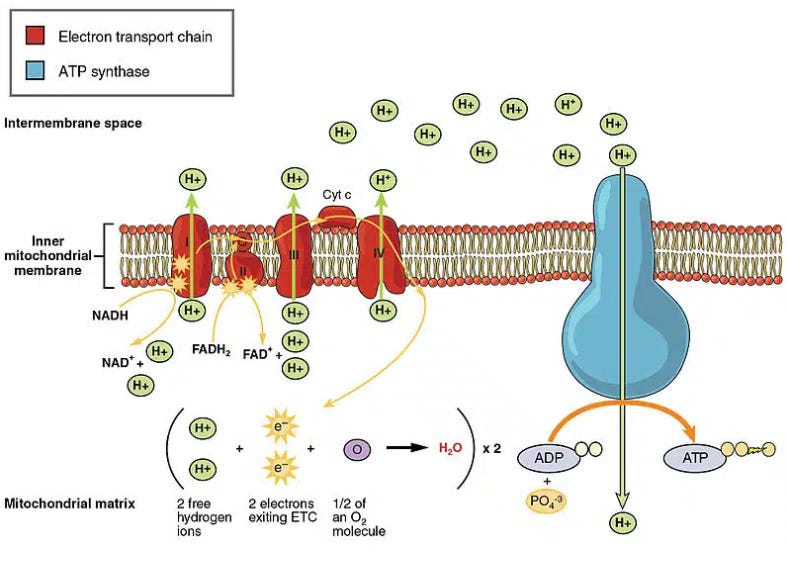
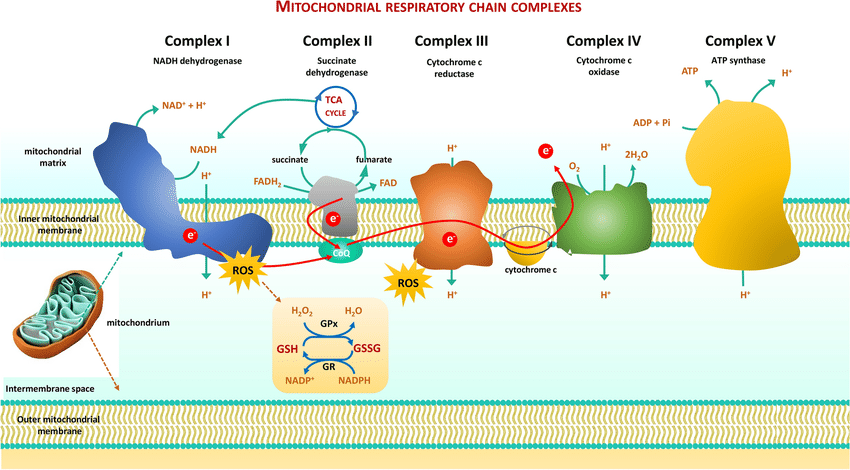
7. The Electron Transport Chain (ETC) — Energy Factory
NADH and FADH₂ deliver electrons to CoQ10 (ubiquinone), then down the chain of complexes (I → III → IV).
This flow drives proton pumps that create a gradient across the inner mitochondrial membrane.
The enzyme ATP synthase (Complex V) uses that gradient to make ATP — the universal energy currency of your cells.
As electrons reach the end, they combine with oxygen to form water, while CO₂ is produced earlier in the Krebs cycle, together signaling efficient oxidation.
8. When Everything Works Right
Glucose and fructose flow smoothly from food → blood → cells → mitochondria → ATP.
CO₂ rises, oxygen is efficiently used, lactate stays low.
The result? Steady energy, warm body temperature, calm nervous system, and strong anabolic hormones.
9. When Things Go Wrong
Glucose or fructose isn’t properly absorbed in the gut, which leads to fermentation and SIBO like symptoms such as bloating and gas.
In the liver, glycogen isn’t properly formed, leading to high circulating glucose.
Insulin release is insufficient, leading to high blood sugar.
If PDH is inhibited or the redox balance is off:
Pyruvate piles up → lactate ↑ (even if fasting glucose is normal)
Mitochondria underperform → ATP ↓
Stress hormones rise to compensate → cortisol ↑, adrenaline ↑
The body feels the drop in energy and blames the carbs, when the real issue is oxidation, not intake.
Why People Think Carbs Are the Enemy
Let’s start with what goes wrong.
Most people don’t oxidize glucose well because their PDH enzyme is blocked and their metabolism is dominated by fatty acid oxidation (FAO).
That’s the Randle Cycle in action, the metabolic tug-of-war between fats and carbs for mitochondrial entry.
When fats win, glucose loses.
High free fatty acids flood the blood (from stress, fasting (even an overnight “fast”), low-carb, or inflammation).
Those FFAs inhibit glucose uptake into a cell (leading to hyperglycemia) and pyruvate dehydrogenase (PDH), the enzyme that lets glucose enter the mitochondria.
Result: glucose isn’t taken up and can’t be oxidized → builds up as lactate → fatigue, brain fog, poor recovery.
The body sees this and panics.
It pumps out cortisol, adrenaline, and glucagon to mobilize even more fat and sugar, creating a stress loop where fat oxidation keeps glucose blocked, and glucose builds up without being used.
This is why people feel “stable” on low-carb: they stop feeding the broken system.
But they’re doing it by raising stress hormones and lowering metabolism, not by fixing the underlying issue.
What This Looks Like in Real Life
You feel energetic but “wired.”
You sleep poorly, wake up hot or anxious at 3 a.m (mostly due to hypoglycemia; this happened to me all the time when my metabolism was broken)
You lose muscle fullness and pump.
Libido drops, SHBG rises.
Labs show high fasting glucose, high HbA1c, but “normal” insulin.
T3 drops, reverse T3 climbs, cortisol stays elevated.
That’s not “fat-adapted.”
That’s stressed adaptation.
Your body has switched from running on clean, oxidative energy (glucose → CO₂ + ATP) to running on emergency mode (fatty acids → incomplete oxidation + adrenaline support).
Low-carb works the same way caffeine does: it stimulates, not heals.
As a disclaimer, burning fat isn’t bad. But avoiding glucose because glucose oxidation is broken isn’t the solution.
Why You Want Glucose Oxidation Back
When glucose oxidation is restored, everything changes.
Hormonal Upgrades
T3 increases → Glucose promotes the conversion of T4 into T3, the thyroid’s active hormone that sets your cellular metabolism.
DHEA-S and testosterone rise → cortisol goes down, and DHEA flows toward androgens instead of stress steroids.
IGF-1 increases → better muscle synthesis, recovery, and youth hormones.
Lower SHBG → more free testosterone availability.
All of this depends on glucose actually reaching the mitochondria and being burned cleanly.
Metabolic Calm
Proper glucose oxidation = high CO₂.
High CO₂ = better oxygen delivery (Bohr effect).
This means: calmer mind, better focus, lower anxiety, deeper sleep.
When oxidation is high, the nervous system finally relaxes. You don’t need caffeine or adrenaline to function.
Physical Performance
When you oxidize carbs properly:
Muscles stay full and strong.
Lactate drops → faster recovery.
Energy feels smooth and powerful instead of spiky.
This is why athletes with efficient glucose oxidation can perform at high workloads on high-carb diets, while others crash trying.
Why Glucose Oxidation Fails
If carbs aren’t the problem… then why do so many people feel worse when they eat them?
Because their metabolic engine is jammed.
The problem isn’t glucose, it’s the pathway that burns it.
When glucose enters the cell, it’s supposed to flow cleanly through glycolysis → pyruvate → pyruvate dehydrogenase (PDH) → mitochondria → CO₂ + ATP.
That’s efficient oxidation. That’s how carbs raise T3, DHEA-S, IGF-1, and drive high energy metabolism.
But when oxidation breaks, that flow stalls. Glucose builds up, gets converted to lactate, insulin spikes, energy crashes, and people blame the carbs.
Here’s what’s really blocking that pathway.
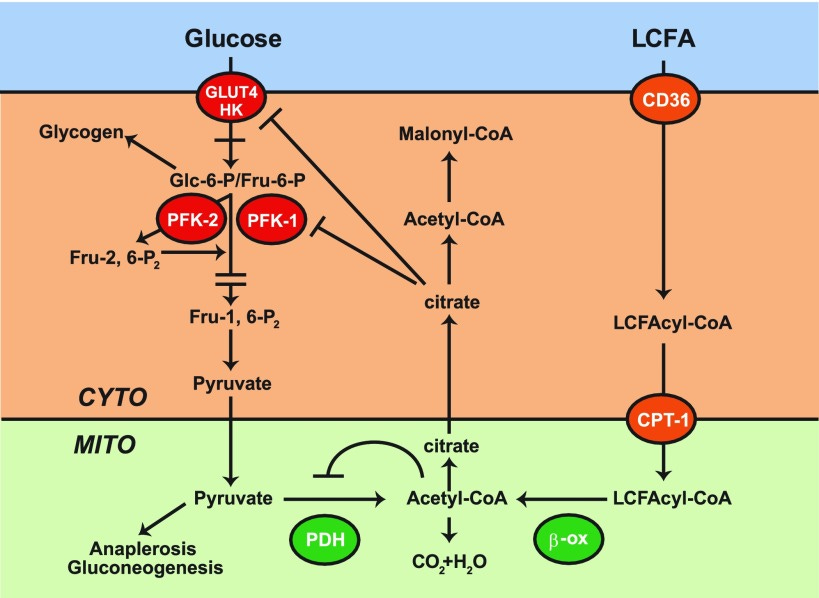
1. Fatty Acid Oxidation Dominance (Randle Cycle)
When fatty acids are being burned at high rates, glucose can’t enter oxidation (this heavily depends on total caloric intake as well).
This is called the Randle Cycle, fats and carbs compete for the same mitochondrial machinery.
High free fatty acids (FFAs) from stress, fasting, or low-carb diets inhibit PDH, the enzyme that allows pyruvate to enter the mitochondria.
PDH inhibition means glucose can’t be oxidized, it just gets recycled into lactate.
That excess lactate causes fatigue, brain fog, and reactive hypoglycemia after carb meals.
So when people eat carbs while FAO is dominant, they experience “carb crashes”, not because of carbs, but because fats are blocking their oxidation.
This is why suppressing fatty acid oxidation (with compounds like Pyrucet, aspirin, or meldonium) can instantly make carbs feel clean again.
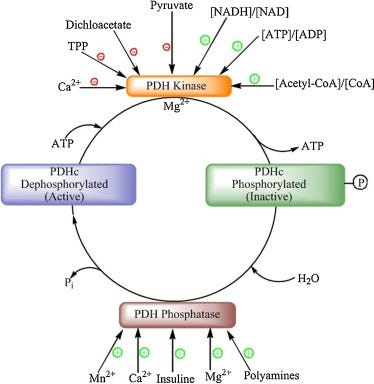
2. PDH Inhibition
PDH (pyruvate dehydrogenase) is the gatekeeper between glycolysis and the mitochondria.
PDH is often shut down by stress or nutrient deficiencies:
PDK (pyruvate dehydrogenase kinase) phosphorylates and inactivates PDH.
Acetyl-CoA excess, high ATP, high NADH to NAD, cortisol, glucagon, and adrenaline increase PDK activity.
Thyroid suppression, low B1, Mg, B2, B3, B5, or ALA deficiency make it worse. In this graph you can see all the nutrients needed and that PDH is quite a complex enzyme complex.
That’s why high-carb diets can only work if PDH is active.
3. Reductive Stress and Low NAD⁺
Even if PDH is open, oxidation still fails if the cell can’t recycle NADH back to NAD⁺.
That’s called redox imbalance, and it’s what traps metabolism in a pseudo-hypoxic, low-energy state.
Low NAD⁺ =
Poor electron transport chain (ETC) function
High lactate and ROS
Sluggish ATP generation
“Tired but wired” energy
Compounds like niacinamide, PQQ, and Pyrucet restore NAD⁺ and push the redox ratio back toward oxidation.
This is also why chronic stress, hypoxia, or inflammation keep you stuck in low oxidation, they drain NAD⁺ and choke mitochondrial flow.
4. Mitochondrial Dysfunction (ETC Bottleneck)
Even with glucose inside the mitochondria, oxidation depends on electron transport chain efficiency.
When Complex I or III slow down, NADH accumulates and electrons leak, creating oxidative stress instead of energy. This increases the demand for antioxidant pathways like superoxide dismutase, hydrogen peroxide and glutathione peroxidase, which is supported by zinc, magnesium, copper, selenium and manganese.
That’s why oxidative support (vitamin K2, methylene blue, CoQ10, succinate, vitamin C) can drastically increase ATP and CO₂ production.
More CO₂ = better oxygenation = calmer nervous system and deeper recovery.
The takeaway:
You can’t just eat more carbs.
You need a clean electron flow — from glucose → PDH → TCA → ETC → CO₂.
5. Gut & Endotoxin Interference
Finally, one of the most overlooked brakes on glucose oxidation is the gut.
Endotoxin (LPS) from bacterial overgrowth or poor bile flow directly inhibits PDH and activates FAO, pushing you right back into the Randle trap.
This is why people think they’re “carb intolerant.”
They’re not, they just have a gut-derived metabolic block.
Fixing digestion (improving bile flow, lowering endotoxin, reducing fermentation) can make previously “intolerant” carbs feel fine again.
The Bottom Line
You can’t burn carbs efficiently if:
Fatty acids dominate (FAO > glucose oxidation)
PDH is inhibited or blocked by stress/nutrient deficiency
NAD⁺ is low and redox is reduced
Mitochondria are sluggish
Gut endotoxin keeps you inflamed
Once you address these, carbs start working again.
The rest of the article is all about how to restore proper glucose oxidation and include solving every step. I’ll show you how to identify which step you need to work on and how to fix it. As well as a 14 day playbook on how to get the ball rolling.